You tie on your running shoes and put in your earbuds, ready for a heart rate-raising run, but you call it quits early because your legs start to ache or become so tired it feels like you can’t take another step. Or maybe you had a great Zumba workout but thirty minutes later your legs are throbbing so badly that only elevating them brings relief.
Many athletes, professionals and amateurs alike, experience some kind of leg pain at one time or another, whether from the mechanics of pounding movement on a hard surface or legs staying in the same position for extended periods. But rarely do they attribute the discomfort to a dysfunction in their venous (veins) system.
However, according to Dr. Cindy Asbjornsen, vein specialist and founder of the Vein Healthcare Center in South Portland, Maine, not all aching legs are simply due to physical activity or even the effects of aging.
“The first thing to understand is that leg pain, in general, is not normal,” said Dr. Asbjornsen. “If your legs hurt after exercise, you should find out why. It could be a build-up of lactic or a pulled muscle, but many folks don’t realize that it may be vein insufficiency that’s causing those symptoms.”
Symptoms of vein insufficiency
Some of the symptoms of vein insufficiency are obvious:
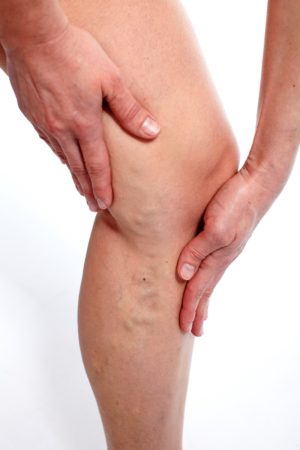
- Visible blue or purple-colored “spider veins”
- Bulging varicose veins
- Open wounds (leg ulcers) on the leg or ankle
Other symptoms are much subtler:
- Achiness
- Swelling
- Itchiness
- Tingling
- Leg cramps after long periods of inactivity or while lying in bed at night
Some people may experience no symptoms at all and some merely accept them as an unavoidable byproduct of physical fitness. But as Dr. Asbjornsen stresses, “you can be in great shape and still have a vein disease that’s developing.”
How exercise impacts veins (and vice versa)
During exercise, your muscles require more oxygen, so veins dilate to increase the volume of blood flowing through the circulatory system. If your veins are not working properly, that means blood can pool in your legs. On the other hand, exercise is beneficial from a venous standpoint because anything that improves pumping blood from the foot and calf muscles back up to the heart is good.
Walking is the best exercise for improving the muscle-pump function, especially following vein treatment. Although walking can help manage the symptoms, it does not prevent vein problems. Neither does exercise cause vein problems, except in extreme cases.
Physical activities that require your legs to support heavier weight over prolonged periods of time, such as weightlifting or backpacking, can put someone at increased risk for developing venous issues.
Repetitive motion sports such as endurance running, cycling and tennis can also put a lot of stress on your leg veins and over time may overcome a normal venous system.
If you’ve got poorly performing veins can it affect your athletic performance? The short answer is yes. If the venous system is not working correctly, then the “extra” de-oxygenated blood (and blood waste products like lactate) can cause discomfort, cramping, fatigue, or other conditions that diminish performance. Even if legs feel great during training, vein issues can also cause legs to hurt after exertion and slow your recovery.
Fixing the problem
If you’ve got a vein problem and certain activities aggravate your symptoms, you can try doing something else. Some people find that swimming, for example, does not produce the same discomfort that running does.
Athletes can live with the problem, but they don’t have to. There are so many options for treatment so that people can continue doing their favorite sports or whatever activity they’re passionate about. They might even see an improvement in their performance.
Modern treatments have excellent initial and long-term success rates when performed by an experienced phlebologist (vein specialist). Endovenous approaches are minimally invasive treatments used to address specific large varicose veins in the legs.
“Endovenous ablation, or EVLA, is considered the gold standard in the treatment of venous symptoms, with success rates between 90% and 98% after five years and has largely replaced previous, more invasive standards of care, such as vein stripping,” explained Dr. Asbjornsen.
Another option for treatment is sclerotherapy, performed either with ultrasound-guidance or with a light-assist, which seals the vein wall of small varicose veins allowing them to fade away.
With both EVLA and sclerotherapy, patients can walk the day of the procedure and return to normal activity, including moderate exercise, within a few days.
If you’re experiencing symptoms of vein disease, Dr. Asbjornsen has a list of 10 things you can do to alleviate your discomfort and help prevent things from getting worse.


Leave A Comment