Guest post by Lesley T. Hoey, DPT
The pelvis, the area of the body people usually refer to as their hips, is an intimate part of the body, yet most people don’t give much thought to how their pelvis and its contents function until something goes awry. Considering there are several medical specialties that, each in their own way, evaluate and treat problems concerning this area of the body, there is value in learning more about its health and function.
The word “pelvis” is a Latin word meaning basin or bucket. It refers to the bony structure, made up of six fused bones, three on each side, that attaches to the bone at the base of the spine called the sacrum. It is also where the legs attach to the body forming the hip joints. It provides protection for the pelvic organs and is an integral part of mobility and stability.
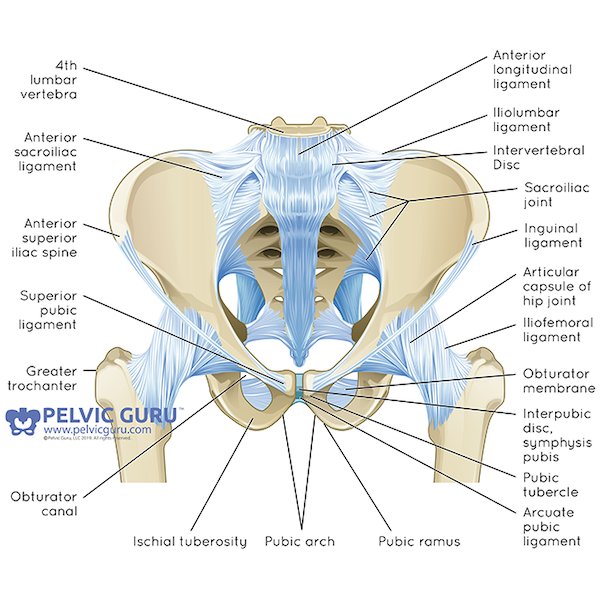
When I meet a person who is coming to see me for the first time for pelvic health physical therapy (PHPT), they typically have lots of questions because their symptoms are not something they typically think of seeing a physical therapist for. After listening to a patient tell the story of their symptoms, a good portion of a first visit may be spent on explaining pertinent pelvic anatomy, what pelvic health PT is, and how it can address their symptoms. Sometimes there is so much to talk about during the first visit a physical evaluation may not happen until the second visit. The evaluation may continue over several sessions to get a full picture of what is going on and all the factors involved.
The specialty of pelvic health physical therapy began in 1977 when Elizabeth Noble, PT started what was called the Section on Obstetrics and Gynecology for the American Physical Therapy Association (APTA). In 1995, the name was changed to Section on Women’s Health to acknowledge the specialized education required to evaluate and treat women’s health needs with physical therapy. In 2011, the name of the section changed again to the Section on Pelvic Health to reflect that men are also affected by pelvic health issues, and PTs learn specialized education and skills to treat them, too.
People are referred to PHPT for a variety of reasons. Some of the more common reasons include but are not limited to:
- urinary/fecal urgency
- urinary/fecal incontinence
- constipation
- pain or discomfort during or after sex
- functional core and pelvic floor training for prenatal/postpartum women
- diastasis recti (an opening or gap in a muscle called the rectus abdominus AKA the 6-pack muscle that can occur during pregnancy)
- pelvic organ prolapse
- functional core and pelvic floor training for men pre/post-prostatectomy
- hernia
- low back or hip pain.
Frequently, people assume their symptoms are normal, even inevitable, assuming “that’s just how it is” or “nothing can be done”. Often people don’t bring up symptoms they are having when they see their primary care provider (PCP), and PCPs don’t necessarily ask about pelvic function during routine visits such as an annual physical. Many suffer in silence because of embarrassment or lack of awareness that services are available that can help change the situation. All the aforementioned symptoms, while common, are not normal pelvic function, and it is possible to improve, perhaps even alleviate, symptoms altogether.
Physical abilities such as breathing, coughing, sneezing, lifting, carrying, postural stability and balance, bladder and bowel control (both containing and releasing the contents without straining) are related to the function and health of deep core muscles in the body.
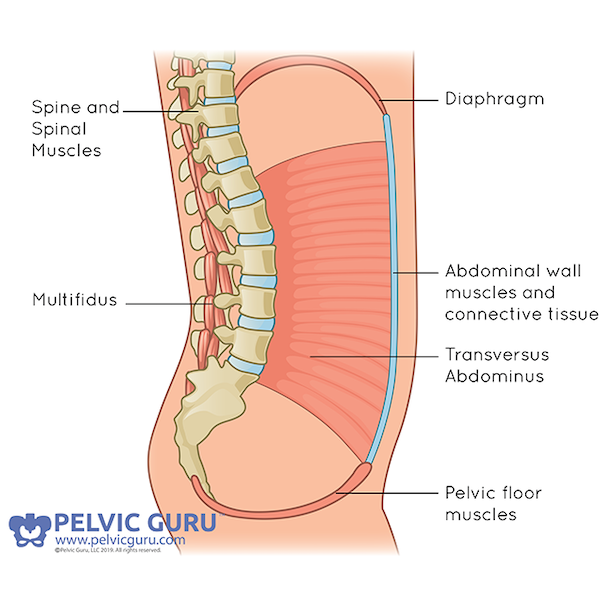
The muscles that make up the deep core are:
- the pelvic floor
- the deepest layer of abdominal muscles called the transversus abdominis
- the respiratory diaphragm
- deep spinal muscles called the multifidi.
These muscles form what is called the “abdominal cylinder”. Together they function to create a system of internal pressure regulation that is integrated into our daily activities without our realizing it because they function automatically below the level of conscious awareness unless something happens to disrupt their function.
For instance, people recovering from COVID may experience problems and challenges with breathing, coughing, bladder and bowel control, and sexual function, and need help improving and recovering their pelvic health and function. Daily activities such as getting up and down from a chair, getting into or out of bed, carrying children, grocery bags, laundry hampers all require the use of the deep core muscles of the abdominal canister. Sexual function, not just the ability to participate but also experience pleasure is affected by the function of the abdominal canister.
These muscles also help support the pelvic organs to help prevent them from sliding out of your body. Childbirth, chronic constipation, poor body mechanics resulting in abdominal bulging with activity and exertion, sedentary lifestyle, jobs that require prolonged sitting can weaken the supportive tone and elasticity of these muscles which can result in a hernia or pelvic heaviness or pressure, a feeling that your organs are sliding or dropping out of your body. Another overlooked function of these deep core muscles is that when they are in good working order they act as a sump pump to improve circulation and clear congestion out of the pelvis, which contributes to a general sense and feeling of physical energy and vitality.
Pelvic health is not just about physiologic function. Orthopedic function of the hips and legs, low back, shoulders, feet, ankles, knees, even the throat, neck and jaw can affect the functional ability of the deep core muscles of the abdominal canister. The pelvic floor and mouth are opposite ends of the same tube running internally through the body; an issue below can be reflected above and vice versa. For example, people with pelvic pain caused by high tone and gripping in the muscles in the pelvic region often have issues with temporomandibular joint syndrome, commonly referred to as TMJ which is characterized by teeth grinding and chronically held tension in the jaw muscles. As above, so below.
Changes in pelvic function may happen suddenly or progress gradually over a period of time for a variety of reasons such as:
- high or low tone in the pelvic floor muscles
- faulty postural alignment and body mechanics
- pregnancy and birth, no matter how long ago (once post-partum always post-partum)
- menopause
- enlarged prostate
- acute or chronic stress
- injury, illness, accidents, surgery
- emotional or physical trauma
- heavy, repetitive physical labor
- extreme fitness training
- medical treatments such as chemotherapy and radiation
- medications such as diuretics, tamoxifen, aromatase inhibitors
This list, while not comprehensive, provides an idea of the multitude of factors that can compromise pelvic function and health.
Research has shown that people don’t often see the utility of this type of treatment. I hope I have succeeded in making the case that PHPT is a highly practical treatment approach for improving and preserving not only pelvic health but overall health. It can also help improve quality of life; not just for the person receiving treatment but for the spouses, family members, and personal hygiene caretakers as well.
While nobody particularly relishes the idea of PHPT, those who come for treatment with a willingness to learn and apply new self management skills notice a difference in the quality of their daily lives. As they become more aware of their symptoms and skilled at managing them they often find, paradoxically, they are less pre-occupied by them. An increase in their agency brings relief. It’s always a joyous and gratifying moment for a pelvic health PT when they hear someone during a breakthrough moment in their treatment exclaim “I wish I had known about this earlier so I didn’t have to live like this!” That is a moment that never gets old no matter how many times we hear it.
Lesley T. Hoey, DPT, is an orthopedic and pelvic health physical therapist and health fitness coach in private practice in the greater Portland area. She got her start in women’s and pelvic health in 2001 by teaching prenatal yoga and helping some of her students give birth. She continued her education in pelvic health after earning her doctorate at the University of New England in 2008. She treats both women and men with orthopedic and pelvic health issues. You can learn more about her and the services she offers at www.drlesleyhoey.com.
Resources
- American Physical Therapy Association (APTA) Section on Pelvic Health website
- Pelvic Guru: An international resource about all things pelvic health for the general public and pelvic health professionals.

Leave A Comment