What’s in a name? Quite a bit believes the Maine Center for Cancer Medicine and Blood Disorders in Scarborough. The practice was founded in 1978 by Dr. Ronald Carroll, Maine’s first medical oncologist. Today the private group practice has 13 cancer specialists on its staff. On any given day they will see from 150 to 175 patients. They also consult on cases across the country.
“We’re not just an oncology practice anymore,” says Dr. Christian Thomas, one of the cancer specialists. “We’re cancer specialists and provide state of the art cancer care to patients in Maine and other states as well. Our reach is more than just regional.”
To better reflect its reach and the level of cancer care it provides, Maine Center for Cancer Medicine decided to change its name to New England Cancer Specialists. A lot has changed in 36 years, not only at New England Cancer Specialists but in the entire field of cancer medicine.
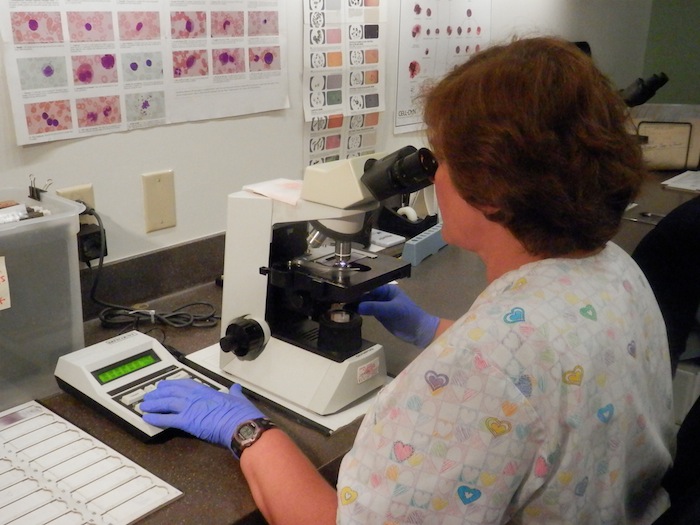
I got a glimpse of some of those changes during a tour of the facility. First stop the laboratory, where they can turn around important blood tests within about 30 minutes instead of several hours. “While the patients are still here the doctors can take those results and deal with them and help the patients rather than sending them home, calling them and bringing them back in,” explained Karen Duncan, one of four medical technologists.
When we walked into the pharmacy I immediately noticed a huge machine and bank of computer monitors against one wall. It’s called the Nucleus machine and it’s where all the drugs are stored. Everything is connected to an electronic medical records system, so that whenever a medicine is moved to the treatment room or one of three satellite offices, it’s logged in and registered. “In the old days,” says Betsy Chase, director of clinical research, “it would get written down and handed to the nurse who would bring it to the pharmacist. In the really old days, the nurses mixed the chemotherapy.”
Not only has the process changed and stringent safety protocols put into place, but the kind of cancer drugs patients get now is also dramatically different. Chemotherapy was first used to treat cancer in the late 40s and today more than 100 drugs are available. Other types of cancer drugs are also being used. Targeted therapy drugs, for instance, which are technically considered chemotherapy, but don’t work in the same ways as standard drugs.
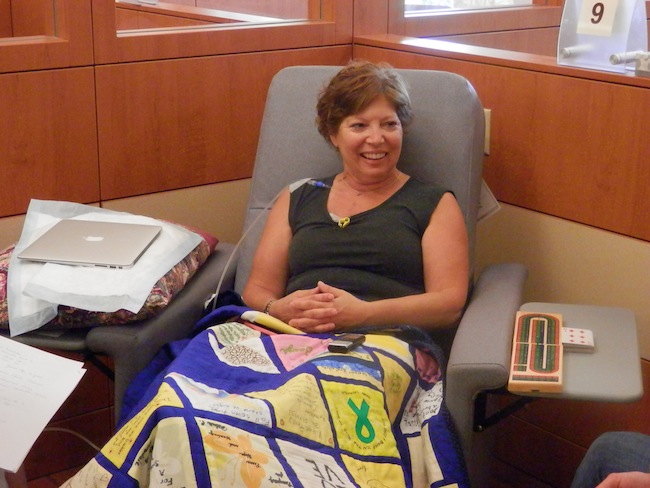
Penny Powell, a lovely woman I spent time with during my tour, is currently receiving standard chemotherapy for stage IV gallbladder cancer. I was diagnosed in February,” she told me. “I come once a week for two weeks and have a week off. I just spoke with my oncologist this morning and basically, it will probably never be cured, but my quality of life will remain good. There are some procedures they’re looking at, but I’ll probably be on chemo for the rest of my life.”
One of the procedures Penny’s cancer specialist is looking at is trans-arterial chemoembolization (TACE). A catheter is threaded into the femoral artery in the groin and up into the hepatic artery, which supplies blood to the liver. “You try to identify which artery feeds the tumor,” explains Dr. Thomas. “You can see that on the x-ray machine and once you identify the artery that feeds the tumor — because there’s always blood flow to the tumor — then you can go into that artery and inject chemotherapy medication. The idea is that now you’re exposing the tumor to a very high dose of chemotherapy as opposed to the rest of the body and then what you can do is seal that artery off. The chemotherapy stays in there and you knock down the blood supply. It’s a double whammy.”
Injecting chemotherapy directly into the tumor is considered targeted therapy. Another new type of cancer treatment is immunotherapy, which uses parts of a person’s immune system to either boost the immune system or attack cancer cells directly.
Penny currently gets chemotherapy intravenously, but that too is changing says Jim Olson, a nurse in the dispensing pharmacy: “Patients can take medication at home, no longer do they have to come in and get a lot of IV medicine. It’s a huge benefit to the patient. The outside is that you need to monitor it very closely. Close communication with the patient is key. That’s something we do very well. Many patients still have to come in for chemotherapy, but the trend now is to go to oral. We’re seeing more and more of it and it really has changed the face of chemotherapy.”
Behind all of the changes in cancer treatments is research. Director of clinical research Betsy Chase says New England Cancer Specialists has about 30 different studies running every year. They do both drug company and government sponsored studies. “The pharmaceutical ones are where you get the new drugs and the government sponsored ones are where they compare existing treatments against each other to see which one is the better one or they’ll do sequencing. Is it better to do radiation, then surgery, then chemotherapy or
A day or a week doesn’t go by without a new type of cancer drug says Dr. Thomas, but when you look at the evolution of cancer care, equally important is how treatment can now be tailored to the individual patient. “We understand cancer now much more as an individual disease and not just as a category,” he says. “We know now how to differentiate patients who have maybe a form of cancer that doesn’t need any treatment. On the other hand, we may have a cancer that is so aggressive we have to treat it immediately and there’s anything in between. If you try to figure out what those differences are, that is where a lot of our research has gone. We’re individualizing cancer treatment based on markers and that allows us to treat patients more appropriately.”
Individualized treatment plans for patients like Penny, who travels three hours round trip for her chemotherapy. She made the choice to be treated at New England Cancer Specialists and says she’s grateful for the care she has received and also for the promise that new therapies may hold. She is determined to be well.




I was diagnosed with multiple myeloma in 2012 stage 4 went to Maine cancer specialists for treatment had bone marrow transplant at Dartmouth was in remission for 4 yrs. I found out n Feb that it’s ting to come back so I am having chemo treatments once as week the cancerspecialists is a great place the Dr nurses and all the staff are great compassionate I
I remember you Diane for sure but I never knew where u went I just wanted You to know my story as the center is good to patients like family
Hi Corinne. I’m glad you found me! I’m sorry to hear that you’re going through this but you’re in good hands. I believe in the power of positive energy and that’s what I’m sending you right now.