Fran Paris, who is 79, has a balance problem and tries to keep herself steady so that she doesn’t fall. When she noticed that Woodford’s Congregational Church was offering a Fall Risk Screening Event to help people learn more about their risks, she hightailed it over there.
high·tail ˈhīˌtāl/verb
1. move or travel fast.
Hightailing it is not a good thing to do if you’re at risk of falling. Neither is forgetting to take your morning blood pressure pill, which Fran did or leaving your cane in the car, which she also did. I know she won’t mind me telling you these things, because just as she learned some lessons from them, so might the rest of us.
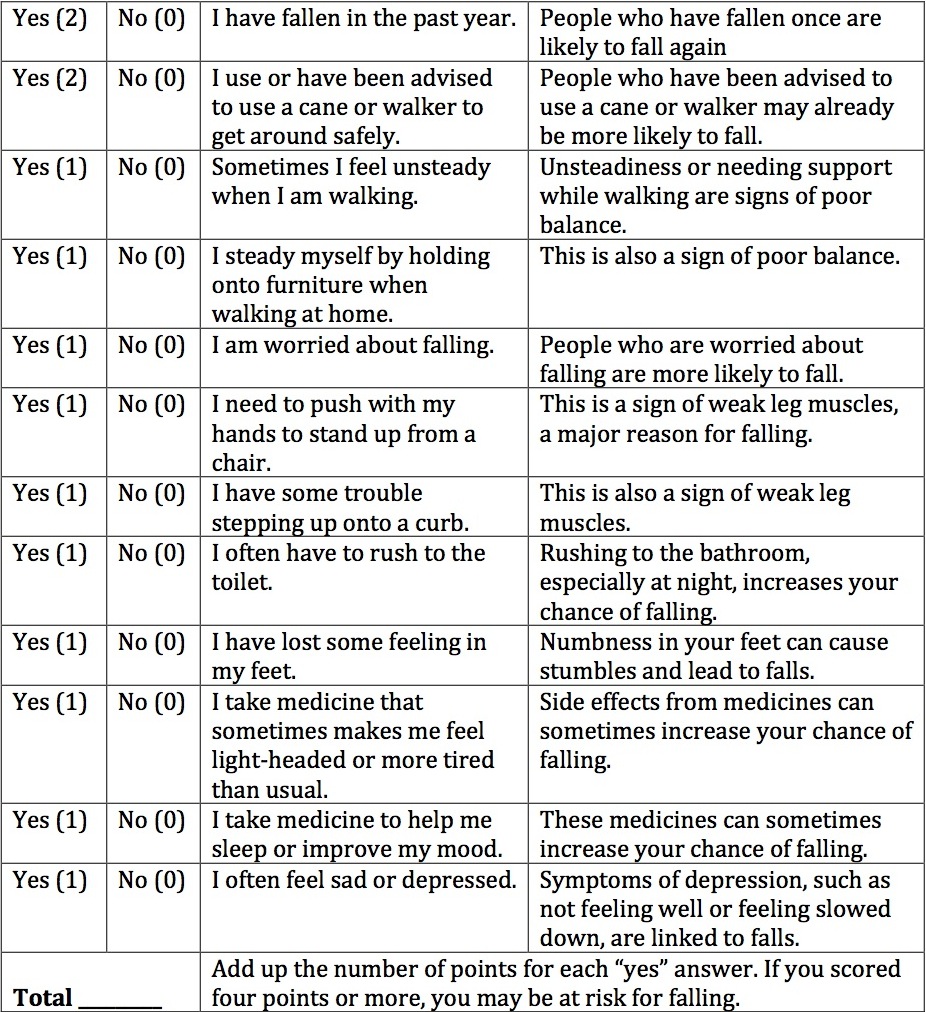
The screening was sponsored by the Southern Maine Agency on Aging, the University of New England, Maine Medical Center and MaineHealth. Fran was gracious enough to let me shadow her as she went through her paces. First thing she had to do was fill out a self-assessment form, which was developed by the Centers for Disease Control and Prevention for its STEADI program. I made a chart with all of the questions so that you can check your own risk.
Check Your Risk For Falling
Circle “Yes” or No for each statement below Why it mattersSource: CDC
If your self-assessment shows that you may be at risk of falling, you should have a conversation with your doctor about how you might lower your risk.
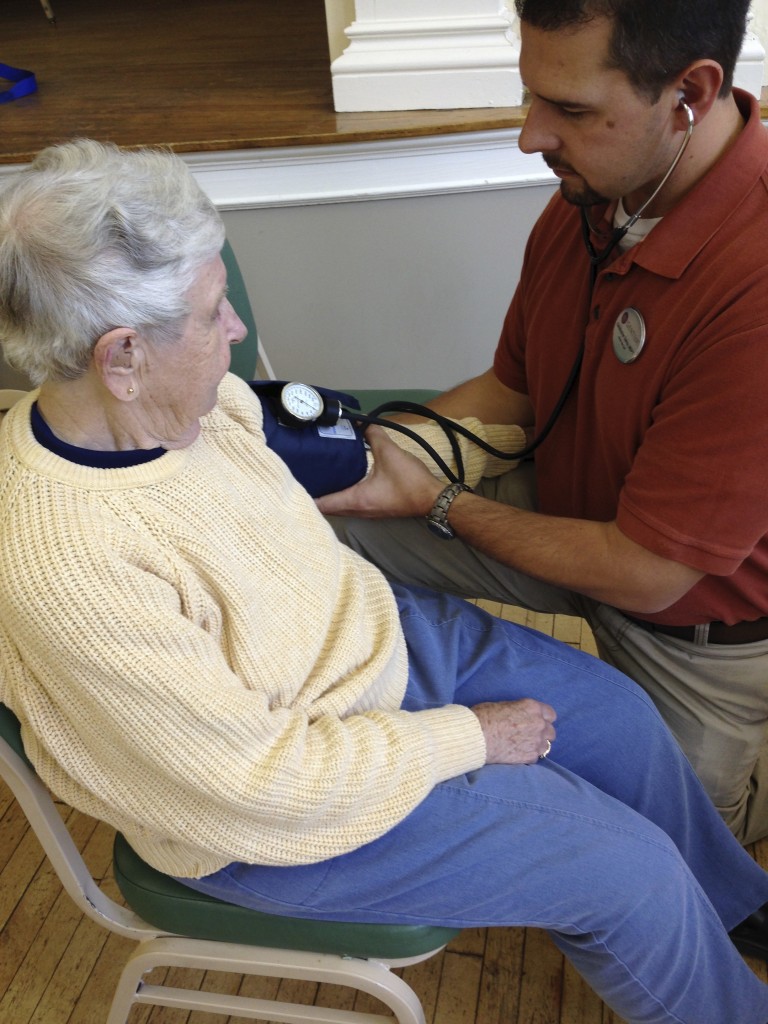
The next step for Fran was to get her blood pressure checked, first while seated and then when standing to see if she had postural hypotension (aka orthostatic hypotension). It’s when your blood pressure drops when you move from lying down or sitting up to standing — a big risk for falling.
Possible symptoms of postural hypotension
- Dizziness or light-headedness
- Feel as if about to faint or fall
- Headaches, blurry or tunnel vision
- Feeling vague or muddled
- Feeling pressure across the back of your shoulders or neck
- Feeling nauseous or hot and clammy
- Weakness or fatigue
When symptoms are apt to happen
- When you stand or sit up suddenly
- In the morning, when blood pressure is naturally lower
- After a large meal or alcohol consumption
- During exercise
- When straining on the toilet
- When you are ill
- If you become anxious or panicky
If you notice any of these symptoms, the first thing you should do is bring them to the attention of your healthcare provider. Fran’s blood pressure was high — not a surprise, but what she didn’t realize is that high or low blood pressure can increase the risk of falling.
Her next task was to pop up out of a chair on the count of three and walk to an orange cone and back. The goal is to make it in less thatn12 seconds. The farther out you are from that time, the greater your fall risk.
Fran’s last test was to see how many times she could get up from a chair and sit down with her hands crossed against her chest. Unfortunately, when her time was nearly up, the movement irritated her back and she decided no more. Patti League, an RN, and wellness specialist at MaineHealth, explained that back pain can be a risk for falling and that it might be a good idea for Fran to do some appropriate exercises to strengthen her back and belly muscles. Again, she should check with her health care provider first.
Before she left, a graduate student from the University of New England’s College of Pharmacy spent time with Fran going over medications that she took. Many medications have side effects or interact with other drugs, which can greatly increase a person’s risk of falling. The CDC says it’s important to talk with your health care provider about your medications, especially about reducing or eliminating the following drugs:
- Psychoactive drugs, especially any benzodiazepines
- Any medications that have anticholinergic side effects
- Sedating OTCs, specifically Tylenol PM (which contains Benadryl) and Benadryl
What did Fran learn about her risk of falling?
One of the most important things Fran learned was that her concern about losing her balance and falling was valid. She has several risk factors, including high blood pressure, a bad back, and some other health issues. She also learned that she should never forget to take her blood pressure medicine and should be using her cane as often as possible. And she discovered that popping up and down out of a chair is not a good thing to do and that she needs to move more slowly and thoughtfully.
Liz Weaver, the Agewell Coordinator at Southern Maine Agency on Aging (SMAAA) says every year around this time they usually do education and awareness events to mark Falls Prevention Awareness Day — last year they did a Flash Mob in Monument Square! This year, they decided to provide screenings in several locations and have had so much success helping people like Fran, they plan to do more. SMAAA and MaineHealth also offer an extremely helpful fall prevention program called A Matter of Balance. Fran is already signed up for the January classes.
If you’d like more information about future fall risk screenings or upcoming A Matter of Balance classes, visit the MaineHealth website or call 207- 661-7120 and ask to speak to someone about fall prevention programs.
Be safe!




Great article and public service, Diane! I shared this one on Facebook.
For your audience:
this former EMT strongly urges that you pay close attention and share this article widely. I’ve been on the scene of many unpleasant and often tragic experiences stemming from a variety of falls and their outcomes.
When I was a kid, I noticed a few habits of elders who lived long and enjoyable lives. Foremost among these habits: walking every day. Of course, there are many good health effects from just taking a walk, but one key benefit is keeping legs strong and practicing balance. That can make a difference when hustling to the bathroom at 2 o’clock in the morning.
The programs Diane mentions here are highly recommended for anyone who has the slightest concern about falls, for friends and family or on their own behalf.
Share this post with all your friends and family!