Anyone can get hepatitis C, but here in the United States, baby boomers — people born between 1945 and 1965 — are five times more likely to be infected. The reason behind the high rate of infection among boomers isn’t completely understood, but it’s believed that most were exposed in the 1970s and 1980s when hepatitis C rates were among the highest.
Some were infected in a healthcare setting — from a blood transfusion, for instance. At that time, we didn’t have universal precautions or widespread screening of the blood supply, says Maura McDonald, a nurse practitioner at Maine Medical Center’s Virology Treatment Center.
Universal precautions were introduced by the CDC in 1985, so things were happening well before 1985. The blood supply was not safe until 1992. Our universal precautions and infection control procedures were not really in place prior to that, so exposure could have happened quite innocently.
Maura McDonald, MPH, FNP-C, MMC Virology Treatment Center
Other boomers may have been exposed because of sharing needles when injecting drugs. It only takes one time.
Even with a safer blood supply, we still see a high rate of hepatitis C. Most newer cases can be attributed to injection drug use. Either way, both baby boomers and people who currently have a substance use disorder are considered at high risk.
Routes of transmission
Hepatitis C is a viral infection that is primarily transmitted through direct contact with contaminated blood. It can be spread in other ways as well.
While rare, spreading hepatitis C through sex is possible. Having a sexually transmitted disease (STD) or HIV, sex with multiple partners, or rough sex appears to increase a person’s risk for hepatitis C. Hepatitis C can also be spread when getting tattoos and body piercings in informal settings or with non-sterile instruments. Some people don’t know how or when they got infected.
CDC
There are vaccines available for hepatitis A and B, which are also caused by viruses, but none is available yet for hepatitis C.
Symptoms
Diagnosis at any age is often missed because about 80 percent of people who are infected don’t develop any symptoms. When they do appear, they may include:
- Fever
- Fatigue
- Decreased appetite
- Nausea
- Vomiting
- Abdominal pain
- Dark urine
- Grey-colored feces
- Joint pain
- Jaundice
Testing for hepatitis C
Hepatitis C can cause serious liver damage, but it often takes decades for it to happen. During that time, people often have no idea they are infected. According to the CDC, “Once infected with the hepatitis C virus, nearly 8 in 10 people remain infected for life. Up to 3 in 4 people who are infected don’t know, so they aren’t getting the necessary medical care.”
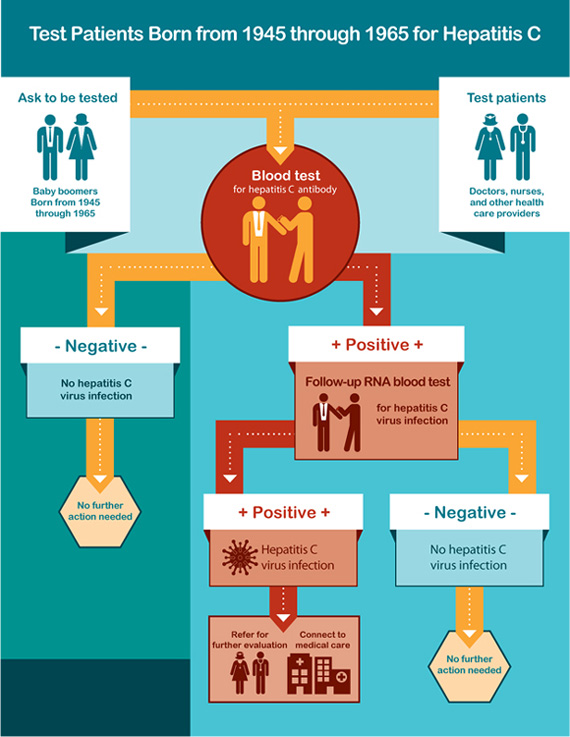
That’s why it’s important to test people who may be at risk. The first step is usually to look for antibodies in the blood. If it’s positive, it doesn’t mean you have hepatitis C, only that you were infected at some point in your life. Once you’re infected, you will always have antibodies in your blood. If your antibody test is positive, you should have a followup test, called an RNA blood test to see if you have an infection that needs to be treated.
When it comes to testing baby boomers, Maura says they’ve been trying to encourage all primary care providers to offer it to their boomer patients, but not all do. I’m in that age group and I can’t recall any doctor ever suggesting that I be tested. If your provider doesn’t say anything, you should. It pays to be proactive.
I certainly have had people in the baby boomer generation come to me with seemingly no risk factors at all and testing positive for hepatitis C. I think we tend to think that it only exists in people with a history of injection drug use, but that’s not necessarily the case.
Maura McDonald
Why it’s important to know if you have hepatitis C
It’s estimated that about 60 to 70 percent of people who carry the virus develop chronic liver disease.
- 5 to 20 percent will develop cirrhosis (scarring of the liver).
- One to 5 percent will die from cirrhosis or liver cancer.
- Hepatitis C is a leading cause of liver cancer.
- It is the leading cause of liver transplants.
Treatment
It used to be that patients with hepatitis C had to be treated with multiple injections of interferon along with a pill called ribavirin. The combination had side effects and came with only a 50-50 chance of a cure.
New medications called direct-acting antivirals have revolutionized how hepatitis C is treated. They are made up of molecules that target specific proteins in the virus and prevent the virus from replicating and causing an infection. They come in pill form and have cure rates of 90 to 100 percent, with fewer side effects and in a much shorter time period.
For those of us who worked in the interferon days, it seems short. Interferon was a good six to 12 months treatment course. Now the treatment course is usually completed within eight to 12 weeks.
Maura McDonald
But Maura says one of the challenges they face is clarifying misinformation, especially about treatment options.
People think the old treatments are still the way to go and the new treatments are really very, very different. And insurance pays for this. Some people don’t realize that if they don’t have health insurance, we’re able to access medications directly from the drug company. It does take a little longer because we need to take a couple of steps, but we can access medication directly from the drug company. So even patients who are uninsured or underinsured, that’s not a showstopper for us.
Maura McDonald
Who should be tested
We’ve discussed two high-risk groups but here’s a longer list of people who may be at risk of hepatitis C and should consider being tested.
- Born from 1945 through 1965
- Have ever injected illegal drugs, even if only once
- Had a blood transfusion or organ transplant before July 1992
- Received blood or clotting factor concentrates made before 1987
- Have been on kidney dialysis for several years
- Are health care or public safety workers who’ve been stuck with a needle or other sharp object with blood from person with hepatitis C or unknown hepatitis C status
- Have HIV
- Born to a woman with hepatitis C
Learn more and spread the word
Maura encourages people to spread the word about hepatitis C. Doing so may help protect the younger generation against developing liver disease in the first place. If a baby boomer was infected a long time ago, she says the hope is they don’t have liver disease now, but if so, it can be managed.
You’ll find more information about hepatitis C (and other forms of hepatitis) on the CDC and Maine Medical Center’s Virology Treatment Center websites.


Leave A Comment