For nearly 30 years — ever since she was about 10 years old — Michelle Spencer endured headaches. Migraines, doctors said.
When she was pregnant with her second child, she passed out cold on a visit to Santa’s Village with her husband and toddler daughter. It can happen during pregnancy she was told.
About four years later, she was on the phone with a friend and suddenly didn’t feel well. Her friend drove over and found her asleep on the bed. For about 24 hours, Michelle couldn’t remember things, like people’s names.
Fast forward to 2000. Her toddler daughter was now in high school and Michelle was getting ready to go to her school concert. “I remember thinking something wasn’t quite right,” she recently told me. “I tried to talk to my husband and he thought I was joking, but then he could see that my words weren’t coming out right. He wanted to take me to the hospital, but I bounced right back and wanted to go to the concert.”
All of these things were warning signs that something bad, really bad, was going on inside Michelle’s head. But because otherwise she felt healthy and led an extremely active lifestyle, she wasn’t that concerned.
The cause of all those headaches
The bomb dropped on October 5, 2014. “We were at a cross country meet,” she says, “my son was running. I was having a fabulous day. We got into the car and were heading home when I suddenly had major pains in my head and I couldn’t tell my husband. He took one look at my face and immediately knew it was more than a headache.”
In the ER at Eastern Maine Medical Center, Michelle had a CT scan and MRI of her brain. And there it was: the cause of her years of miserable headaches and unexplained “spells.”
Michelle, who is now 40, was born with a tangle of abnormal blood vessels in her brain and all that time, they weren’t carrying blood back and forth from her heart to her brain as they should and they were ballooning under the pressure.
There’s a name for the tangle: Arteriovenous malformation or AVM — a rare condition that happens in less than one percent of the general population. An AVM can develop in blood vessels throughout the body but is more apt to happen in the brain or spine.
The cause is unknown, but as it was in Michelle’s case, AVMs are usually congenital.
AVM symptoms
An AVM may not cause any signs or symptoms, but if it does, they may include:
- Seizures
- Headache or pain in one area of the head
- Muscle weakness or numbness in one part of the body
Some people (like Michelle) have more serious symptoms:
- Severe headache
- Weakness, numbness or paralysis
- Vision loss
- Difficulty speaking
- Confusion or inability to understand others
- Severe unsteadiness
In retrospect, Michelle fit the classic picture for an AVM. According to the Mayo Clinic, “Symptoms may begin at any age but usually, emerge between ages 10 and 40. Brain AVMs can damage brain tissue over time. The effects slowly build up and often cause symptoms in early adulthood.”
The biggest risk of having a brain AVM is that it will rupture and bleed into the brain.
That’s exactly what happened to Michelle Spencer. “The neurologist at EMMC could see that not only did I have an AVM on the left side of my brain, but it had burst.”
Arrangements were made for her to be transferred to Tufts Medical Center in Boston for brain surgery. Because the weather was bad, she couldn’t be airlifted. The four and one-half hour ambulance ride was hell — mostly for her family. Michelle was on morphine for the pain and at that point, her memory was nearly gone.
“I was very close to death, “she explains. “If I had a major stroke in the ambulance there is nothing they could have done to prevent it. My family was frantic. One of my biggest upsets is that my children and husband had to go through so much. My kids didn’t know whether I’d be coming home.”
At Tufts, they didn’t rush her into the operating room. Instead, they stabilized her with medication for nearly two weeks. “In the meantime,” she says, “I could walk and talk although I didn’t always make sense. There were certain words I couldn’t say and I would often use “pen” and “envelope” to replace words.”
On October 16th, Michelle had a procedure called embolization to seal off the abnormal blood vessels and reduce the risk of more bleeding. The next day she underwent eight hours of brain surgery to completely remove the AVM.
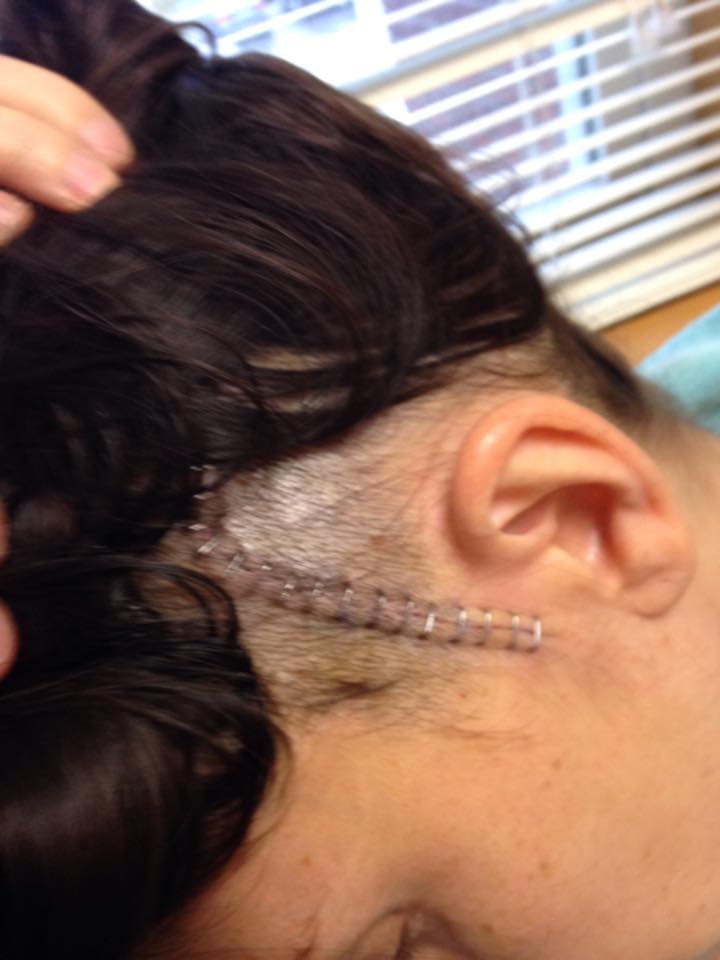
“I had 44 staples in my skull,” she exclaims.
She went home October 21, four days after her brain surgery. On the 25th, she attended her son’s track meet. “This is where it all happened after my son’s race,” she says. “I went on the 25th to watch him again and took this picture.”
AVM treatment
Michelle needed embolization and surgery because her AVM ruptured and bled into her brain. Once that happens, the risk is high that it will happen again and so the AVM must be treated says UCLA neurosurgeon Dr. Neil Martin. In addition to surgery and embolization, AVMs can also be treated with focused, stereotactic radiation therapy. Dr. Martin describes the treatment of AVMs in a 38-minute UCLA YouTube video.
Surgery may not be necessary for all AVMs, which Dr. Martin also addresses in the video. The key, he says, is assessing the risk of it rupturing and bleeding into the brain.
Healing
Until hers was discovered, Michelle had never even heard of an AVM. It may no longer exist in her brain, but the after effects continue to linger.
“My vision has been impaired right from the beginning,” she says. “In both eyes, I can see from the middle to the left but not to the right. I still have memory issues and I’m still having speech therapy. And I do get tired, but more in my eyes and mental capacity and not physically. The surgeon says it can take up to two years before it’s as good as it’s going to get.”
She sometimes struggles with depression, anxiety and pain, as many people do after an AVM or brain injury. She sees it as a “normal thing due to injuries” and prefers exercise, essential oils and reiki treatments to medications.
Michelle’s life before her AVM ruptured was jam packed: “I have two beautiful kids 18 and 15 and a husband of almost 21 years. I have been a dancer, Curves manager, fitness instructor, fitness center manager, Tai Chi instructor and senior adult worker.”
Her experience may have slowed her down, but it didn’t stop her in her tracks. “I have wanted to get back to work even as I had staples in my skull.” (She’s now teaching a senior fitness class four hours a week.)
An update
I first wrote about Michelle in May 2015. Two years have passed since her surgery. They haven’t been easy years.
In honor of AVM awareness month, I asked her to give us an update.
“The past year has been a struggle. Since July 2015, I have had severe pain (headaches, but not regular headaches), fatigue, blurry vision, and dizziness. When all of the issues take place, my memory fails.
Most of the issues are made extremely worse if stress is a factor and I have learned that when you have a brain injury, your stress levels are more severe than an average individual.
I’ve learned also, that someone with a brain injury has a different outlook and also is seen in a different way by others (even their friends, family, etc.) I know that it hasn’t been easy for my husband or my children to have our lives changed so dramatically. They were used to being taken care of in every way. It is after the long haul that you find the true loves in your life — whether it be family or friends. A life altering health concern is not for the weary.
I have visited the normal medical model doctors like neurologists, pain management, ER attendance. I’ve had CT’s, MRI’s, EEG, etc., and haven’t gotten any answers to the questions I continue to ask.
Due to extreme pain, I was told that I have nerve pain due to my surgery itself and the scar tissue on the inside and outside of my brain. I asked if it was going to be a long term or life long ordeal and I was told that the doctors hope not. The blurry vision and dizziness were diagnosed as vertigo but my vertigo isn’t treated by the average visit to a Physical Therapist.
Some of the above all go together. Again, I have been told I have strange migraines that include: dizziness, nausea, blurry vision, headache and the memory issues. These are the bad times. Bad times can last for a few hours, a few days ,or a cluster of a couple days a week for a month or so. During those times, it affects my life and the things I want to do.
I also have great days. Days when I feel pretty good. I have the energy to do the things I enjoy which are working, hiking, taking care of my great niece and watching my son run races with a wonderful community of teammates, friends, and parent collaborators.
I believe I have found the middle ground. I had to find it on my own and not get it from a doctor as a diagnosis. On days that I know I just don’t feel great, I need to rest, which probably has been the hardest lesson I have learned.
Until now, I have thought if I allow myself to rest, I am allowing the devil called AVM to win. But, now I believe I am just giving myself a deserved break and then can get up and fight again.”
Even with the challenges she faces, (along with her family and friends) Michelle says the most about thing is that she is alive to even tell her story.





This story causes me to marvel at modern medicine — the research, studies, and technology — and the strength of human beings who have the courage to face life-threatening issues. Sometimes a little bit of hope is all we need to hang onto. Michelle and her family found the strength to hang on. I wish them all the best.
Another great story, Diane. Thanks for sharing this…you just never know who else might benefit from knowing about AVMs.
Wow! Hits way to close to home. It took them 6 years to discover I was having seizures. What else are they missing?
I want to say I suffer from migranes with botox treatment I can deal I am very happy for u and your family u finally got answers and relief.congrats .you are brave………….love Erica
My husband was diagnosed in 2009 with trigeminal neuralgia caused by an avm deep in his brainstem. In 2013 the avm ruptured causing a severe stroke and traumatic brain injury. He is now in a wheelchair but fighting hard everyday to get out of it. He lost his hearing and vision on his left side We take life one minute at a time !!
Wow – interesting information. My migraines were a side effect from brain surgery for Epilepsy, so I sure wish there was something to treat that! 😛
I have had bad migraines since about the age of 10. They are everyday and really are getting unbearable. I am going to a neurologist and a psychiatrist because of them. My Neurologist is trying nerve block shots in the back of my cerebellum. She does want me to get an MRI, and after Dianes story I am.
My sister-in-law had this. She had migraines for years. The dr and hospital NEVER gave her a mri or cat scan. If they had she would be alive today. Its a horrible thing. When my daughter was having migraines all the time we insisted she had a mri, the dr did, but she didnt have it thank god!
My mothers AVM caused life long permenate damage and will never be the same. This lady sounds lucky! They are scary for sure. I wish I could have my mother back how she was, but thankful to still have her.
I suffer daily from chronic migraines and they’ve never found the reason why.
So reading your story was extremely scary as I get like that, a few times a week (slurred speech, blurred vision, sharp head pains, auras, etc…) and I’ve suffered for 33 years, I’m 44 years old with 2 wonderful boys 3 and 15. 🙂
I also have horrible memory problems and I’m on daily medication (Topamax 400mg ).
Thanks for sharing your story.
Wow! So glad she came through this ordeal.
I also had an avm . it started out as a noise in my head that was maddening at times. I also had very severe vertigo, falling at times. I went to many Doctors before a radiologist in Asheville, N.C. found my problem during an arteriogram. I will forever be grateful to Dr. Kennedy! I was referred to Emory University hospital where they were able to embolize it. Although I had to have it embolized twice,
I was able to avoid brain surgery and have no side effects, other than some noise in my head.
I’m glad this lady is recovering, but doctors should have been consulted after she started having those episodes and CAT scans and then MRI’s should have been done until they found the reason for them. If they had ballooned enough to rupture they would have been found before lasting damage had happened.
I’m happy you got treatment and you found out the cause of the headaches I’m time. I also was diagnosed with a rare brain tumor 15, May 2014. I am living in guyana and they didn’t have the facilities here to undergo surgery and I was referred to dr. Jeffrey Florman at maine med. Through my ordeal I found life can be snatched away in a blink of an eye. I’m only 23 and I would love to continue living my life as normal. But this experience has really given me a new meaning to life. I would ish you all the best and you have the most important part of your life with you, your family. . God bless you
This story is so similar to mine. I had my AVM removed on February 17,2014. I had never heard of an AVM and am forever grateful for all the doctors, nurses and staff here in Charlotte thay basically saved my life. It started with one headache that was so painful that I visited my primary doctor. He recommended I get a CAT scan done, which is when I found out I had an AVM that burst . After being in hospital for a week , I was told it was highly recommended that I get it removed. It was in an operable spot and much larger than most AVM’s. A few weeks later, I had an embolization and a cranium done by some of the best surgeons around. I am extremely lucky to have just minimal side effects (memory loss, vision loss). It’s been a year and half and d I’m still on medication but am grateful for every day in alive. I’m so happy to hear Michelle in is doing well ! It is a very scary thing to go through, especially when you have children and don’t know if you’ll be there for them the next day.
My son, at 12 years old, had a ruptured AVM. We had never heard of it before. He had 2 types of treatment… surgery to remove the cluster, but because they could not remove all of it, they followed up with Gamma Knife Radiation. He is now 19, a Dean’s-List college sophomore, plays sports, and is as active as if it never happened. None of this was by luck or coincidence. The only thing that saved his life was prayer… and those answered prayers included an exceptional neurosurgical team, great medical care, divine connections, and a complete healing. Not a day goes by without being reminded of the miracle God gave us, and we are truly grateful.
Thank you for sharing your story Kathy. It gave me goosebumps. You have so much to be grateful for and to be proud of.
We have been battling migraines for a p years. My hubby had epilepsy as a baby until six years old. Migraines as far back as he can recall yet none of the doctors seem to think the migraines are related to the epilepsy. Avm has been noted in all his ft scans and MRIs going back 7 years yet neurologist says no connection. We are finally getting in to see the neurosurgeon in october and I hope he sees the correlation.
Best of luck to you and your husband. I hope he gets an accurate answer and appropriate treatment.