
Deep vein thrombosis is a blood clot that develops deep in a vein, usually, but not always, in your leg. The biggest risk with DVT is that a piece of the clot could break off and travel through your bloodstream up to your lungs, where it might cause a blockage or pulmonary embolism. A big enough clot can be deadly. Even a small one can cause long-term problems.
Dr. Cindy Asbjornsen, a vein specialist at Vein Healthcare Center in South Portland, says that about 60 to 100,000 Americans die every year from DVT or pulmonary embolism (PE). It’s the pulmonary embolism, not the DVT that kills them. Of that group of people, 10 to 30% will die within a month of their diagnosis. That’s why it’s important to know risk factors and symptoms.
DVT risk factors
Hypercoagulation
Some people’s blood is considered hypercoagulable. When we cut ourselves, the blood coagulates or forms a blood clot to stop the bleeding. That’s a good thing. It becomes risky if your blood is hypercoagulable or clots too much. Common causes of hypercoagulation are:
- Genetics
- About 5% to 8% of the general population are genetically predisposed to forming blood clots
- Certain conditions or diseases increase the risk of developing clots, including
- Pregnancy
- Cancer
- Heart disease
- Other factors
- Birth control that contains estrogen
- Hormone replacement that contains estrogen
- Age
- Obesity
- Smoking
Stasis
In this case, stasis means that your blood is either flowing too slowly or not at all. Stasis can happen if you sit for hours on end — at your desk or on a plane, for instance. It can also occur in someone who is in the hospital or confined to bed.
Damage to the walls of a blood vessel
The classic situation is if you have an accident, where you actually damage vessels enough to see bruising. Another cause is if you have surgery and blood vessels are actually cut. Anytime the walls of a vein are damaged, it can predispose you to clotting.
Dr. Cindy Asbjornsen, Vein Specialist, Vein Healthcare Center
COVID
In some people with COVID, the virus causes a significant inflammatory response that can damage the walls of veins and cause blood clots. Research is ongoing, says Dr. Asbjornsen.
More research is coming out literally daily, but one of the bigger review studies showed that people with COVID who were in the sicker groups, people in the ICU or certainly hospitalized, were at a much higher risk for clotting than people who had milder cases.
Dr. Asbjornsen
DVT symptoms
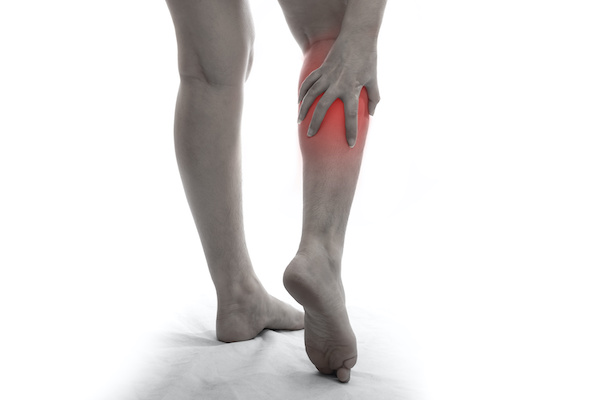
- Pain
- Tenderness
- Swelling
- Discoloration
- Skin that is warm to the touch
You may have no symptoms with DVT, but the big one to be on the lookout for is swelling. If DVT is suspected the gold standard for making a diagnosis is ultrasound.
Pulmonary embolism symptoms
If you have a clot that causes a blockage in your lung, it will likely cause these symptoms:
- Difficulty breathing
- Chest pain that gets worse when you take a deep breath or are lying down
- Coughing or coughing up blood
- A heartbeat that is irregular or faster than normal
If you have any of these symptoms, don’t waste any time getting medical attention.
Treating DVT
In 2012, my sister-in-law Donna was undergoing cancer treatment and developed a blood clot in her leg. A piece of it broke off and made it to her lungs. Fortunately, she survived the ordeal but had to be on blood thinners for six months and wear compression stockings.
Blood thinners
When Donna was treated, people on blood thinners tended to be prescribed Coumadin or Warfarin. Today, there is a whole new line of medications. They’re called direct action oral anticoagulants. Many people find them easier to tolerate because it’s not necessary to have regular blood tests to monitor blood levels and regulate the dosage.
They’ve become much more common, but they tend not to work as well with certain types of blood disorders. The reason being which part of our clotting cascade they actually act on. So, they’re great, but they haven’t made coumadin and injectables like heparin obsolete yet.
Dr. Asbjornsen.
Compression stockings
If you need compression stockings, your doctor should tell you the appropriate stocking weight. If not, ask.
A millimeter of mercury reading dictates how much compression you need. Normal compression amounts can be 20 to 30 or 30 to 40. Sometimes it will be lower than 20 for just a casual travel sock, but in the realm of venous disease 20 to 30 is the general starting point.
Dr. Asbjornsen
The key with compression, Dr. Asbjornsen says, is not just how much squeeze you get, but also that the garment fits well. It may take some trial and error to find the right fit, especially if you are very short or tall. Persevere!


Also, when you hear about compression stockings do you immediately think of thick ugly beige ones? These days, your head might spin at the design choices. Donna had to start wearing them again recently and was determined they wouldn’t be black, white, or beige. She’s happy with the whimsical selection she found at a medical supply shop near her home.
Yes, they’re excellent. I have to wear them day and night. I like them a lot!
Donna, my sister-in-law
Final piece of advice
What’s most important for people to know about DVT and PE, says Dr. Asbjornsen, is that if you have a pain in your leg that you can’t explain or some unusual swelling, get it checked out. If you’d like to learn more about DVT, she recommends the website Stop the Clot.

Oh yes, definitely do not waste any time with lung pain and irregular heartbeat! Call 911, get an ambulance. Don’t try to drive yourself in, as long as you live in an area where and ambulance can get there in minutes. Or even Lifeflight. The people transporting you have all kinds of equipment and training to save your life if things go downhill quickly, which they can.