Malignant melanoma is a serious, sometimes deadly form of skin cancer. You might think that sunscreen would protect you. Here are two reasons why that isn’t necessarily so:
1. People slather it on and then bake in the sun twice as long as they should.
2. Some sunscreens are not broad-spectrum. In other words, they protect against UVB rays but not UVA rays, which may also cause skin cancer — including malignant melanoma.
Sunscreen guidelines for manufacturers
- In order to claim that sunscreen protects against skin cancer, a sunscreen must be at least SPF-15 and must protect against UVB and UVA. If the claim can’t be made, a warning must be added to the label: “This product has not been shown to prevent skin cancer or premature skin aging.”
- No sunscreen is really waterproof so only the term water-resistant can be used and only if studies prove that the product retains its value after being exposed to water.
- The term sunblock can no longer be used because no sunscreen can completely block the sun.
Even if you choose the right kind of sunscreen, you also have to use common sense.
Sunscreen guidelines for us
- Don’t put on sunscreen and then stay in the sun so long you get a sunburn.
- If your skin starts to get red or feel uncomfortable, don’t just reapply sunscreen, cover up, or get in the shade.
- Wear protective clothing, a hat, and sunglasses along with sunscreen.
The goal isn’t to avoid getting any sun exposure at all. In fact, sunlight is an important source of Vitamin D. The recommendation is that we get from five to 30 minutes of sun exposure between 10 am and 3 pm at least twice a week to our face, arms, or back. What you don’t want to get is sunburned. You especially want to protect your children’s skin.
Sunburns are risky
Research shows that the incidence of malignant melanoma has increased more than six times over the past 40 to 50 years. Several studies have shown a strong connection between getting sunburned during childhood and adolescence and developing malignant melanoma.
Several years ago, Dr. Frederick Aronson, who is now retired, but at the time was an oncologist at New England Cancer Specialists talked with me about the risk.
Most of the ultraviolet radiation that causes melanoma is delivered to the individual at risk before age 20. There are migration studies that show if you grow up in a high sun region and moved to a lower sun region in your 20s, your melanoma risk is as if you lived in the high sun region all your life and vide versa. If you live in a low sun region and move to a high sun region in your 20s your melanoma risk remains relatively low.
Dr. Frederick Aronson, Retired Cancer Specialist
Mike Cushman’s melanoma story

Mike Cushman was diagnosed with advanced malignant melanoma in 2010. Sadly, he passed away on September 3, 2013, but his story continues to be important because it might save someone else’s life. He first shared it with me in 2012.
I had a suspicious mole on the back of my head under my hair. My daughter spotted it and suggested my doctor check it out. The biopsy came back benign. A short time later, I felt a lump in that same area. It was removed for biopsy and came back malignant melanoma. I cannot trace the melanoma to my family. I seem to be the only one. As a child growing up in the 50s and 60s I probably had my share of sunburns.
Mike Cushman
Treating malignant melanoma
The most effective treatment for malignant melanoma is surgery. Depending on a variety of factors, chemotherapy, radiation therapy, and immunotherapy may also be used.
Mike had what is known as a BRAF mutation, which can cause normal cells to become cancerous. He participated in a clinical trial of a therapy that targeted the mutated gene, but unfortunately, it didn’t work for him. He was then put on a drug called Yervoy, which pitted his body’s immune system against the cancer cells, but by then it had spread to his liver and bones. When we last spoke, he’d had two out of four treatments. He said there was a 20 percent chance the drug would stop the melanoma from spreading more, but it was too early to tell if it was working, and he wasn’t “overly excited.
I’m tired and nauseous, having a rough time right now — typical chemo side effects. But, I’m still here, I’m still functioning.
Milke Cushman
Even though he clearly didn’t feel well, Mike was more than happy to talk with me and share his message, which is powerful.
If you find a suspicious mole, get it checked. Don’t let it go. If I’d acted earlier, I would have made out a lot better than I am now.
Mike Cushman
Typical signs of melanoma in a mole
- Asymmetrical shape — one half doesn’t match the other
- Borders are irregular — ragged or blurry edges or pigment that spreads into the surrounding skin
- Color is not even — usually shades of brown, black, and tan, but sometimes white gray, red, pink, or blue
- Diameter — usually bigger than a pea, but can start tiny and get bigger
- Evolving appearance — a change that happens in just weeks or months.
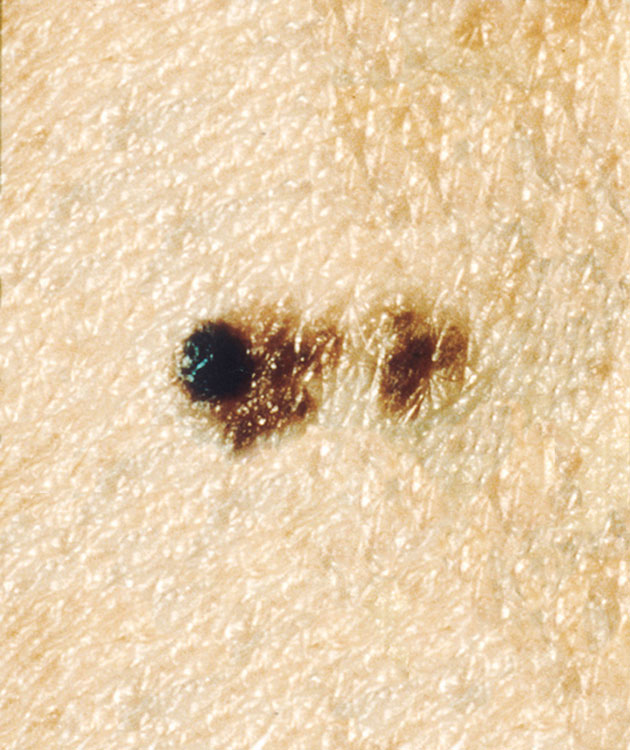
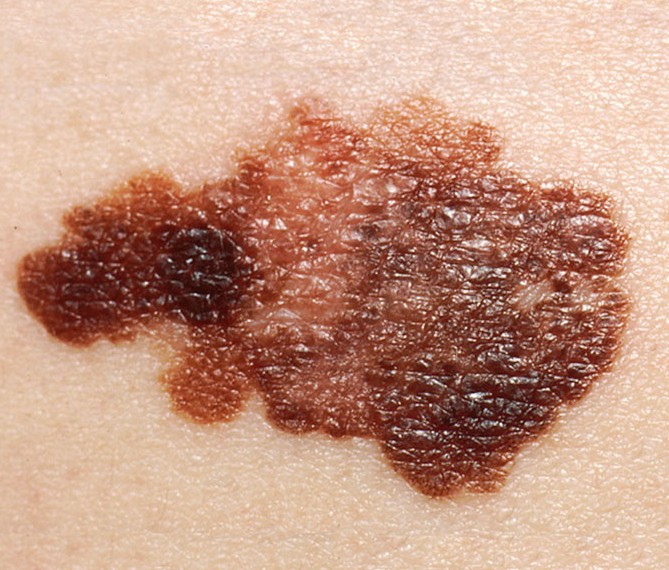
What malignant melanoma might look like
Mike told me he chose not to dwell on any sunburns he got when he was younger, but he certainly learned some hard lessons later on.
I cannot go back and undo the past. What I would have done differently is talk to my doctor about follow-up care with a dermatologist. I am very thankful that my daughter brought to my attention the suspicious mole on the back of my head. My two daughters now have a family history of melanoma and they see a dermatologist at regular intervals. Believe me, I ask them if they have been going to their appointments.
Mike Cushman
Please, follow Mike’s advice. If you have a suspicious-looking mole, get it checked. Now.


Have had quite a journey with dermatology the past couple years. Busy specialty in the Portland area. Finally found a home, I think.
Too many sunburns before age 20 – we had “tanning lotion” and that was it. One neighbor swore by peanut oil — LOL nah, I don’t think so. Blistered my face with that stuff.
Glad to hear, though, that moving to California in my mid-20s wouldn’t have added appreciably to my risk. The sun there was truly intimidating to this pale-faced Yankee! Got used to it, though, and was smart enough to avoid sunburns for the most part.
Baby oil was my go to, but when I noticed my first wrinkle in my late 20s, at least I started covering up my face.